
PATIENT ESTIMATION — patient payment estimator
Give patients a clearer view of financial responsibility
When patients don’t know in advance what they will owe, it’s difficult for them to plan to pay — and it may even cause them to delay care. That’s where a proven patient payment estimator comes in.
Waystar’s HFMA Peer Reviewed Patient Estimation solution sources enriched benefit data to generate highly accurate estimates. Empower your staff to confidently discuss costs upfront, improving point-of-service collections while offering a more transparent and positive patient experience.
Patient Estimation by the numbers

WHAT MAKES WAYSTAR DIFFERENT
Automated, accurate patient payment estimator
When it comes to patient estimates, accuracy matters. We continuously test and improve our patient payment estimator, and we don’t water-down our accuracy rates by excluding the things that are outside our — or your — control. Waystar automates the process of calculating a patient’s liability without manual intervention, improving staff efficiency.
Features + benefits
- Automated real-time eligibility using EDI and RPA
- Out-of-network benefits and estimation
- Easy-to-understand, user-friendly estimates
- Unparalleled scalability
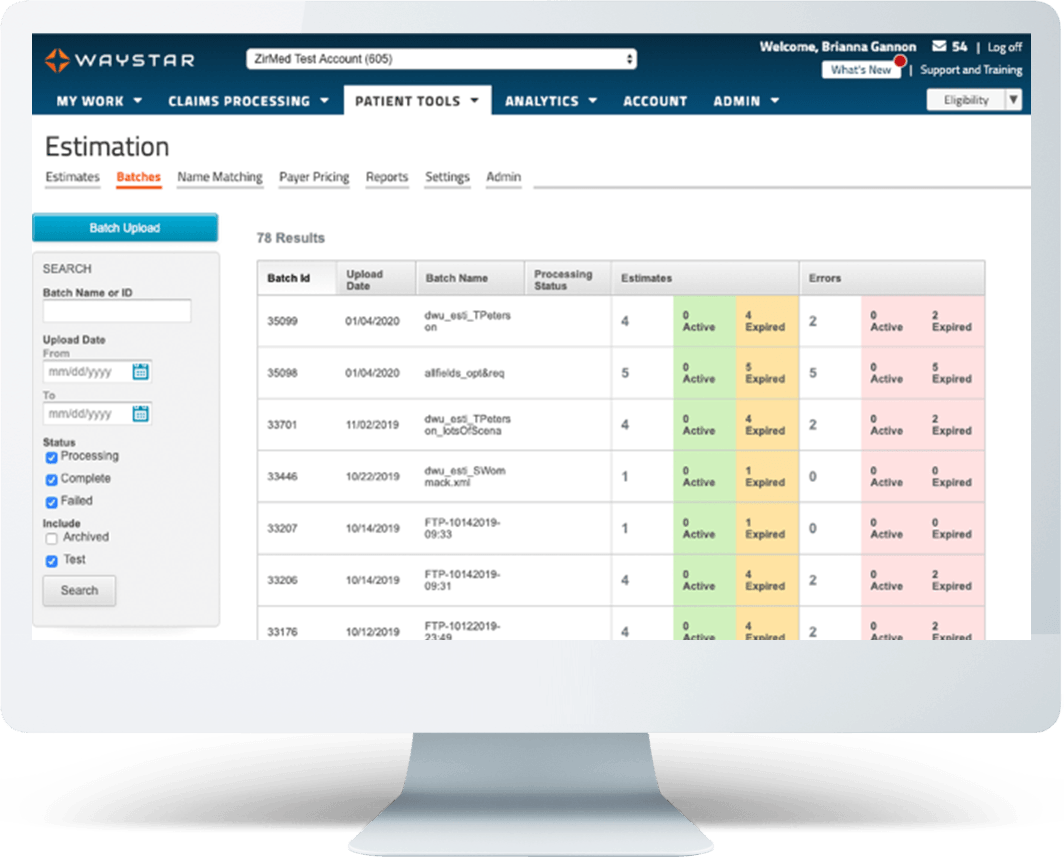

Get greater insight into Waystar’s patient payment estimator
Value that grows with your organization
Discover even more ways to improve your patient experience while collecting faster and more fully. Healthcare organizations across the country are seeing success with our Patient Estimation solution, together with solutions that complement our patient payment estimator:
COMPLEMENTARY SOLUTIONS
Eligibility Verification | Advanced Propensity to Pay | Price Transparency | Claim Management

Speak to a Patient Estimation expert today
If you’re ready to transform your patient experience, increase collections, and reduce bad debt, fill out the form below and we’ll reach out to you shortly. We look forward to talking through your patient payment estimation challenges and opportunities.