A previous version of this blog post was published in May 2020. This version was updated to reflect the telehealth landscape a year later.
Telehealth adoption exploded in 2020 in the wake of the COVID-19 pandemic as many patients were unable or reluctant to seek on-site care. The combination of relaxed regulations and expanded payment parity for appointments made virtual meetings easier and more attractive for providers, who are turned to these technologies to stay engaged with patients—and maintain cash flow. As Dr. Robert McLean, a former president of the American College of Physicians said, “this crisis has forced us to change how we deliver healthcare more in 20 days than we had in 20 years.”
At Waystar, we’ve been closely monitoring claim trends and have witnessed the growth in telehealth firsthand. In fact, the volume of telehealth claims on the Waystar platform grew by more than 100X from March 2020 to May 2020. On two days in late April 2020, they accounted for more than 15% of our total daily claim volume. Before COVID-19, they would have accounted for less than 1%. While restrictions have loosened in 2021 and people have started to venture back out, we expect that telehealth is here to stay. It may not maintain the volume that it did during the height of community shutdowns, but it will certainly remain higher than pre-pandemic levels. Patients became accustomed to the convenience of telehealth for certain kinds of care, and are likely to expect that same convenience moving forward.
For many providers, this shift will require new revenue cycle strategies to meet growing patient demand without overwhelming clinicians and administrative teams—or already strained operating budgets. It’s important to remember this is still very much an evolving care delivery model with the opportunity for errors on the part of both payers, providers, and administrative staff. For this reason, rev cycle professionals should diligently monitor claims to ensure proper adjudication, identify learning opportunities, and uncover areas for operational improvement.
Below, we’ve listed six core telehealth-related metrics you should regularly track to ensure billing accuracy, maximize payer reimbursement, and reduce claim rejections and denials. For more on how to best navigate the evolving telemedicine landscape, check out our resource hub here.
To report on telehealth-related claims, you’ll first need to identify and isolate claims containing telehealth procedure codes. See CMS’ telehealth code list to identify the specific procedure codes and modifiers that apply to your organization.
Payer analysis
1. Payer telehealth claim rejections by volume and/or billed amount
2. Payer telehealth claim denials by volume and/or billed amount
If your telehealth claims are being denied or rejected, do you know which specific payers are doing so at the highest rate? Drill down to discover the specific reason codes payers are attaching to rejections and denials so you can better understand payer-specific rules and avoid these oversights in the future. In some cases, you may identify trends that warrant a call to the payer to correct.
Provider analysis
3. Telehealth claim volume by provider
Review this claim volume by individual provider. If you notice providers within your organization generating a much lower volume of telehealth claims than peers, perhaps they could benefit from additional training on telehealth technology and use cases.
Ensuring billing accuracy
4. Telehealth claim rejections by biller/team
5. Telehealth claim denials by biller/team
Are certain billing personnel or teams producing higher denial or rejection rates than others? Keep a close eye on these trends and remember most of this is new for everyone. If some team members are seeing more rejections or denials than they should, it could be a great opportunity to hold training and collaborate on strategies for success.
Maximizing reimbursement
6. Telehealth claim volume by procedure code
Which telehealth codes are you using? Each code reimburses at a different rate, so choosing the wrong ones could leave money on the table. Be sure to read up on CMS’ requirements (check out their fact sheet and code list) to ensure you’re choosing the appropriate code(s) on each telehealth claim.
Waystar Analytics
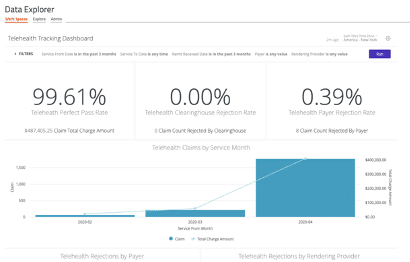
You have all the data you need to drive informed decision making and improve financial performance—you just need the right analytics tool in your corner. Waystar Analytics + Reporting offers a pre-built telehealth dashboard that can help you easily interpret and share all the metrics above, and more.
![6 telehealth rev cycle metrics to track right now [updated]](https://s45903.pcdn.co/wp-content/uploads/2021/05/AdobeStock_547698188-scaled-e1729776946779.jpg)