TeamHealth’s way forward
Managing denials at scale requires more than manual effort. TeamHealth is leveraging automation and AI to streamline appeals, reduce rework, and shift toward proactive denial prevention.
Complexity requires smarter automation
With operations spanning thousands of hospitals and payers, TeamHealth faces significant complexity across claims, contracts, and requirements.
“Our model is pretty complex, understanding all the different payer requirements in 50 states,” said Charlie Brown of TeamHealth.
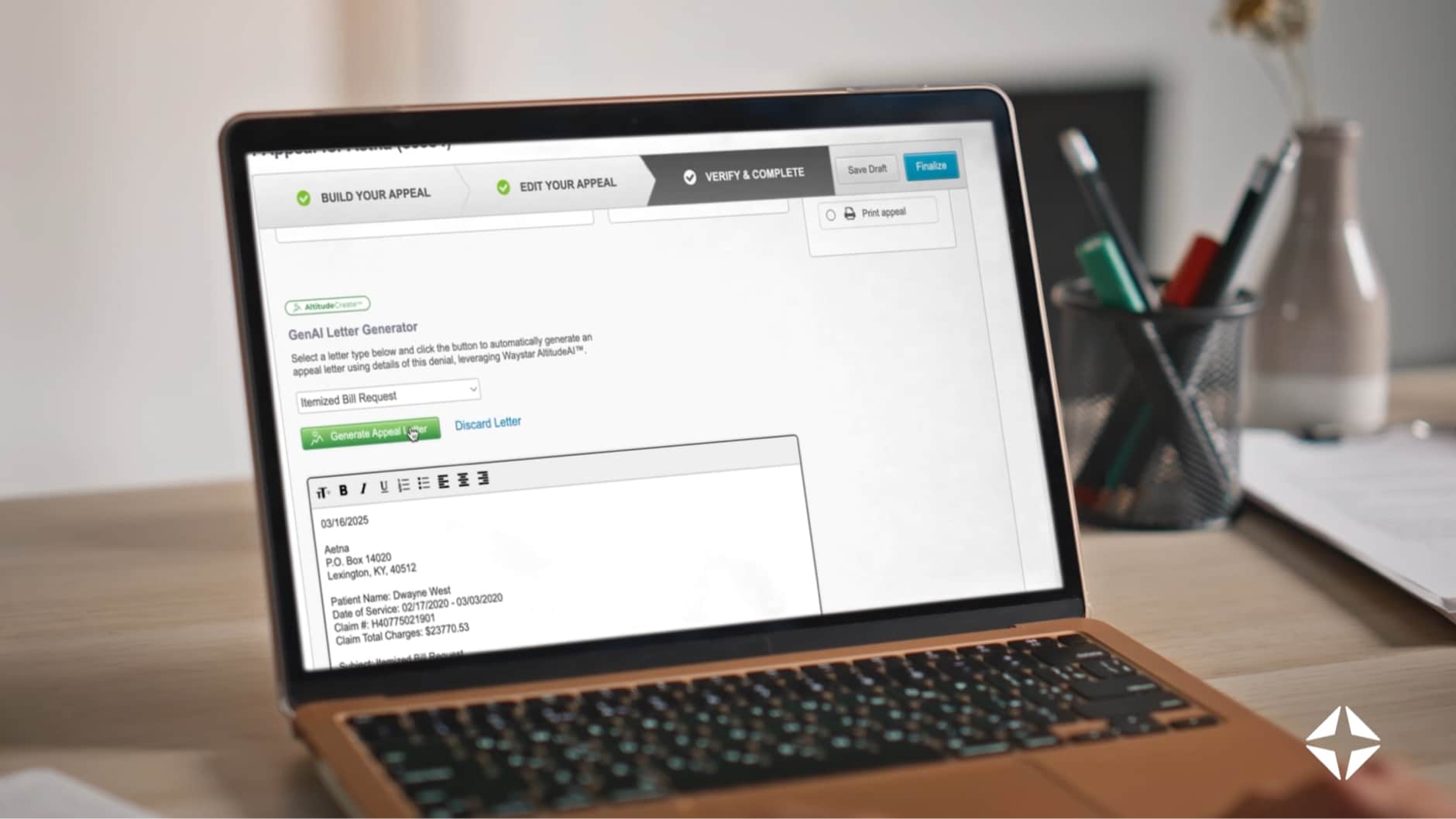
To manage that complexity, automation has become essential. TeamHealth is moving beyond manual workflows by adopting AI-powered appeal letter automation — improving efficiency and closing the feedback loop faster.
“Appeal letter automation has been huge for us… how can we close the feedback loop [and] be more proactive of denial prevention versus reaction,” Brown said.
Driving measurable impact with AI
With Waystar’s automation tools, TeamHealth is seeing meaningful improvements in both productivity and financial performance.
“We’ve seen a 50% productivity increase and 38% revenue lift in those appeals that we’re able to overturn.”
As denial complexity grows, organizations that embrace automation and AI will be better positioned to scale operations, reduce manual work, and accelerate revenue recovery.
Learn how Waystar can help you transform denial management with AI-powered automation.